Prostate biopsies, guided by transrectal ultrasound, require precise CPT coding for accurate billing and reimbursement. Koelis’ technology impacts this process,
and ongoing trials are evaluating biopsy routes.
What is a Transrectal Ultrasound Guided Prostate Biopsy?
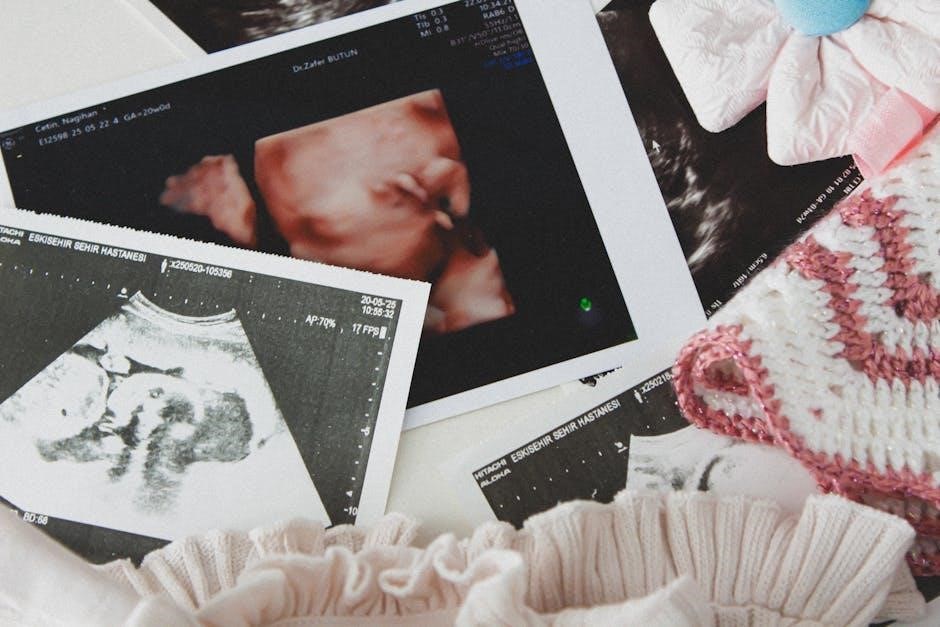
A transrectal ultrasound guided prostate biopsy is a procedure used to diagnose prostate cancer. It involves inserting an ultrasound probe into the rectum to visualize the prostate gland. Core needle biopsies are then taken from suspicious areas, guided by the ultrasound images.
This technique allows urologists to obtain tissue samples for pathological examination, crucial for determining the presence and grade of any cancerous cells. The procedure is commonly performed when a patient has elevated prostate-specific antigen (PSA) levels or abnormalities detected during a digital rectal exam.
Koelis’ MRI-ultrasound fusion technology enhances the precision of this biopsy, improving the detection of clinically significant cancers. Understanding the procedure is fundamental to proper CPT coding.
Why is Accurate CPT Coding Crucial?
Accurate CPT coding for transrectal ultrasound guided prostate biopsies is paramount for several reasons. Correct coding ensures appropriate reimbursement from insurance payers, preventing claim denials and revenue loss for healthcare facilities and physicians.
Furthermore, precise coding supports accurate data collection for tracking healthcare utilization and outcomes related to prostate cancer diagnosis. With advancements like Koelis’ MRI-ultrasound fusion guidance, coding complexity increases, demanding meticulous attention to detail.
Incorrect coding can also lead to legal and compliance issues. Maintaining up-to-date knowledge of CPT guidelines and payer policies is essential for avoiding audits and penalties.
CPT Codes for Transrectal Ultrasound Guided Prostate Biopsy
Key CPT codes include 55870 for the core needle biopsy and 55871 for image guidance, often used together, especially with technologies like Koelis.
55870: Core Needle Biopsy, Prostate
CPT code 55870 specifically describes the procedure of a core needle biopsy of the prostate. This encompasses the acquisition of tissue samples for pathological examination, crucial for diagnosing prostate cancer or other prostatic abnormalities. The code represents the fundamental act of sampling the prostate tissue itself.
It’s important to note that 55870 doesn’t inherently include image guidance; that’s a separately reportable service. The clinical indications for utilizing this code are typically elevated Prostate-Specific Antigen (PSA) levels, abnormal digital rectal exams, or suspicious findings on imaging studies;
As advancements like MRI-ultrasound fusion guidance (such as Koelis technology) become more prevalent, the need for precise coding remains paramount, even though the core biopsy itself is still represented by 55870.
55871: Image Guidance for Core Needle Biopsy of Prostate
CPT code 55871 represents the image guidance utilized during a core needle biopsy of the prostate. This code is not billed independently; it’s an add-on code to 55870, reflecting the enhanced precision offered by imaging modalities. Common modalities include transrectal ultrasound (TRUS) and, increasingly, MRI-ultrasound fusion guidance, pioneered by companies like Koelis.
The purpose of image guidance is to improve the accuracy of sample acquisition, targeting suspicious areas identified on imaging. When MRI-ultrasound fusion is employed, it allows for a more detailed visualization of the prostate, leading to more accurate biopsies.
55871 is appended to 55870 when these imaging techniques are used to direct the biopsy needle, ensuring optimal sample collection.

Detailed Breakdown of CPT Code 55870
CPT 55870 covers the core needle biopsy of the prostate, a crucial diagnostic procedure. Accurate coding is vital, especially with evolving guidance technologies like Koelis’.
Indications for Using CPT Code 55870
CPT code 55870 is indicated when a patient presents with elevated prostate-specific antigen (PSA) levels, suggesting potential prostate cancer. It’s also utilized for individuals experiencing abnormal digital rectal exam (DRE) findings, warranting further investigation. Patients with suspicious imaging results, such as those identified through MRI, are also candidates for this biopsy procedure.
Furthermore, 55870 is appropriate for those with a history of prior negative biopsies but continue to exhibit concerning clinical or radiological features. Ongoing clinical trials, exploring transperineal versus transrectal routes, influence biopsy decisions. The need to characterize indeterminate prostate lesions also justifies the use of this code. Ultimately, the decision to proceed with a biopsy is based on a comprehensive evaluation of the patient’s risk factors and clinical presentation.
What is Included in the 55870 Code?
CPT code 55870 encompasses the entire process of a core needle biopsy of the prostate, performed under transrectal ultrasound guidance. This includes the ultrasound examination itself, guiding the needle placement to target suspicious areas. It covers all needle insertions required to obtain adequate tissue samples for pathological analysis.
The code also accounts for the local anesthetic administration necessary for patient comfort during the procedure. Importantly, 55870 does not include image guidance services provided by technologies like MRI-ultrasound fusion (Koelis), which require separate coding (55871). It also doesn’t cover complex pathology or additional procedures performed during the same session.

Detailed Breakdown of CPT Code 55871
CPT 55871 reports image guidance during prostate core biopsies, often utilizing MRI-ultrasound fusion like Koelis technology, enhancing targeting accuracy and sample acquisition.
Image Guidance Modalities (Ultrasound, MRI Fusion)
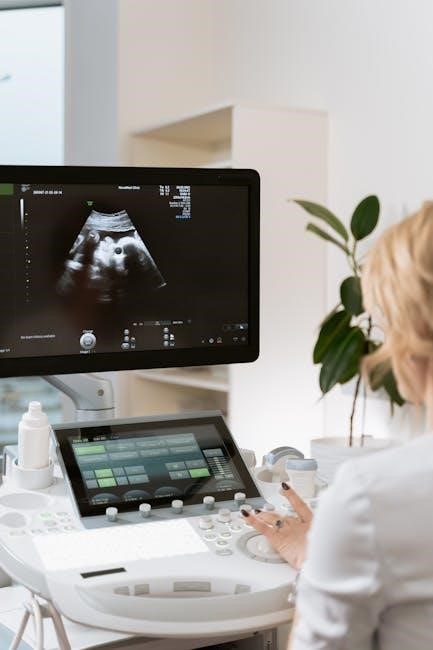
Image guidance for prostate biopsies encompasses several modalities, with transrectal ultrasound (TRUS) being the traditional standard. However, advancements have led to the integration of magnetic resonance imaging (MRI) with ultrasound, notably through technologies like those developed by Koelis.
MRI-ultrasound fusion allows for real-time visualization of the prostate, combining the anatomical detail of MRI with the dynamic imaging capabilities of ultrasound. This fusion guidance significantly improves the precision of biopsy targeting, particularly in identifying suspicious lesions previously detected on MRI.
The use of MRI fusion is becoming increasingly prevalent, driven by clinical trials evaluating transperineal approaches and the desire to enhance diagnostic accuracy. Accurate coding reflects the complexity and sophistication of these image-guided techniques.
When is CPT Code 55871 Added to 55870?
CPT code 55871, representing image guidance, is appropriately appended to 55870 when utilized during the core needle biopsy of the prostate. This addition signifies that technology beyond standard TRUS was employed to enhance targeting accuracy.
Specifically, 55871 is added when MRI-ultrasound fusion guidance, such as that offered by Koelis, is implemented. This fusion combines pre-operative MRI scans with real-time ultrasound imaging, allowing for precise lesion targeting.
The use of image guidance is increasingly common as clinical trials explore improved biopsy techniques, like the transperineal route. Proper documentation demonstrating the use of image guidance is crucial for accurate billing and reimbursement.
Modifiers Commonly Used with Prostate Biopsy CPT Codes
Modifiers -59 and -26 are frequently used with biopsy codes. -59 denotes distinct services, while -26 identifies the professional component of the procedure.
-59: Distinct Procedural Service
The -59 modifier is crucial when multiple procedures are performed during the same encounter, specifically when the procedures aren’t typically billed together. In the context of a transrectal ultrasound guided prostate biopsy, this often arises when additional services, beyond the core biopsy (55870), are rendered.
For example, if a separate lesion is targeted and biopsied, requiring a distinct approach or location within the prostate, -59 clarifies that this isn’t simply an extension of the initial biopsy. Proper documentation is paramount; the medical record must clearly demonstrate the distinct nature of each service. Without adequate justification, claims utilizing -59 are prone to denial.
Accurate application of -59 ensures appropriate reimbursement for the urologist’s complete work, reflecting the complexity of the procedure and the additional skill involved.
-26: Professional Component
The -26 modifier signifies the professional component of a procedure, specifically the physician’s work involved in the transrectal ultrasound guided prostate biopsy. This encompasses the urologist’s skill, expertise, and interpretation of the ultrasound images, as well as the actual performance of the biopsy itself.
Often, facilities bill a technical component (TC) for the equipment, supplies, and facility costs. The -26 modifier ensures the physician is separately reimbursed for their professional services. Correct coding requires understanding whether the facility bills TC and if the physician is reporting the professional component.
Accurate application of -26 is vital for appropriate reimbursement, reflecting the urologist’s cognitive and procedural contributions to the patient’s care.
Billing Considerations & Reimbursement
Detailed documentation is essential for successful claim submissions related to prostate biopsies. Avoiding common denials requires precise CPT coding and adherence to payer guidelines.
Documentation Requirements for Accurate Billing
Comprehensive medical records are paramount for justifying the CPT codes billed for a transrectal ultrasound guided prostate biopsy. This includes a clear indication of the medical necessity for the procedure, supported by PSA levels, digital rectal exam findings, and any prior imaging results.
Specifically, documentation must detail whether a standard biopsy (55870) was performed or if image guidance (55871) was utilized, such as MRI-ultrasound fusion guidance offered by companies like Koelis.
The report should explicitly state the number of cores taken, the locations targeted, and any complications encountered. Furthermore, if modifiers like -59 or -26 are appended, the rationale for their use must be clearly articulated within the documentation to prevent claim denials and ensure appropriate reimbursement.
Common Claim Denials and How to Avoid Them
Claim denials for prostate biopsies frequently stem from insufficient documentation supporting medical necessity or improper coding. A common error involves billing 55871 without clearly demonstrating the use of image guidance, like MRI-ultrasound fusion technology from Koelis.
Denials also occur when the documentation doesn’t justify the use of modifier -59, indicating a distinct procedural service.
To avoid these issues, ensure the medical record explicitly details the clinical indications, the specific guidance modality employed, and the rationale for any modifiers used. Staying abreast of ongoing clinical trials evaluating transperineal versus transrectal approaches is also crucial, as coding may evolve with new evidence.

Transperineal vs. Transrectal Biopsy & Coding Implications
Urologists await clinical trial results comparing transperineal and transrectal prostate biopsy routes, potentially influencing CPT code selection and reimbursement strategies for both approaches.
Coding Differences Between Transrectal and Transperineal Approaches
While CPT codes 55870 and 55871 are frequently utilized for both transrectal and transperineal prostate biopsies, subtle coding nuances exist; The transrectal route, traditionally more common, generally employs these codes as standard practice when image guidance is used.
However, the transperineal approach, gaining traction due to infection risk mitigation, may necessitate careful consideration of code application. Documentation must clearly reflect the technique used, as it can impact reimbursement;
Specifically, the complexity of the transperineal approach, often requiring specialized equipment and potentially longer procedure times, doesn’t automatically translate to a different primary CPT code. Accurate coding relies on detailing all services rendered, including any additional imaging or procedural steps.

Future Trends in Prostate Biopsy & CPT Coding (as of 02/13/2026)
MRI-ultrasound fusion guidance, like Koelis technology, is evolving coding practices. Ongoing clinical trials assessing transperineal biopsies may lead to future CPT updates;
Impact of MRI-Ultrasound Fusion Guidance (Koelis Technology) on Coding
Koelis, a leader in MRI-ultrasound fusion technology, significantly impacts prostate biopsy coding. While the core biopsy code (55870) remains fundamental, the addition of image guidance (55871) becomes crucial when utilizing Koelis systems. This fusion guidance enhances targeting accuracy, potentially leading to more precise biopsies and improved cancer detection rates.
Coders must accurately document the use of MRI-ultrasound fusion to justify the addition of 55871. Proper documentation should detail the pre-biopsy MRI acquisition and its integration with real-time ultrasound during the procedure.
As technology advances, staying current with coding guidelines is essential. The increased precision offered by Koelis may influence future coding updates related to targeted biopsy techniques;
Ongoing Clinical Trials and Potential Coding Updates
Current clinical trials are actively comparing transrectal and transperineal prostate biopsy approaches. The results of these studies, anticipated to be available soon, could influence future CPT coding guidelines. If transperineal biopsies demonstrate superior outcomes, new or modified codes might emerge to reflect the procedural differences and associated resources.
Furthermore, advancements in imaging and guidance technologies, like those from Koelis, may necessitate coding revisions.
Payers are continuously evaluating the clinical and economic value of new technologies.
Coders should monitor industry publications and coding updates from organizations like the AMA to ensure compliance and accurate billing for prostate biopsy procedures.
