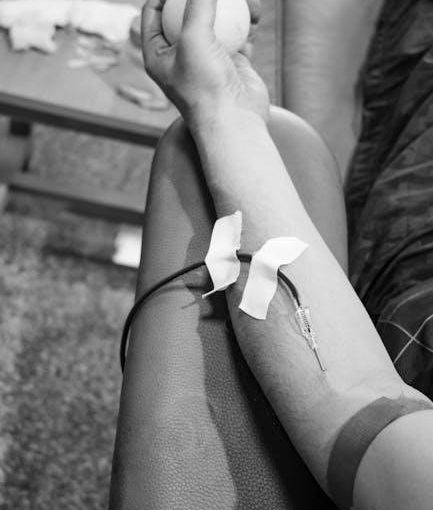
Phlebotomy is a crucial healthcare profession focused on drawing blood for tests, transfusions, research, or therapeutic purposes.
Phlebotomists play a vital role in the diagnostic process, ensuring accurate sample collection and patient comfort during procedures.
Accurate blood collection is paramount; errors can lead to misdiagnosis, incorrect treatment, and compromised patient care outcomes.
What is Phlebotomy?
Phlebotomy, derived from the Greek words “phlebos” (vein) and “tome” (to cut), is the practice of making an incision into a vein to obtain a blood sample. Historically, it was used for bloodletting as a therapeutic treatment, but modern phlebotomy is almost exclusively diagnostic.
Today, phlebotomy is a cornerstone of modern healthcare, facilitating a vast array of diagnostic tests. These tests help physicians monitor patient health, diagnose diseases, and assess the effectiveness of treatments. The process involves skilled technique to minimize patient discomfort and ensure sample integrity.
Essentially, phlebotomy bridges the gap between a physician’s order and the laboratory analysis needed for informed medical decisions. It’s a vital, yet often unseen, component of patient care, demanding precision and adherence to strict protocols.
The Role of a Phlebotomist
Phlebotomists are highly trained healthcare professionals responsible for the collection of blood samples from patients. Their duties extend far beyond simply drawing blood; they are patient advocates and crucial members of the healthcare team.
A phlebotomist’s role includes verifying patient identities, explaining procedures to alleviate anxiety, and meticulously labeling and preparing specimens for laboratory analysis. They must adhere to strict safety protocols, including universal precautions, to protect both themselves and patients.
Furthermore, phlebotomists often assist with point-of-care testing and maintain accurate records of blood draws. Excellent communication and interpersonal skills are essential, as they frequently interact with patients who may be stressed or apprehensive about the procedure.
Importance of Accurate Blood Collection
Accurate blood collection is the cornerstone of reliable diagnostic testing and effective patient care. Even minor errors in the collection process can significantly impact test results, leading to misdiagnosis and potentially inappropriate treatment plans.
Incorrect specimen volumes, improper tube order of draw, or inadequate mixing of additives can all compromise sample integrity. These inaccuracies can necessitate repeat blood draws, causing patient discomfort and increased healthcare costs.
Therefore, meticulous attention to detail, adherence to standardized procedures, and a thorough understanding of pre-analytical variables are paramount. The phlebotomist’s role in ensuring specimen quality directly influences the accuracy of laboratory data and ultimately, patient outcomes.

Essential Equipment & Supplies
Phlebotomy requires specialized tools, including needles, tubes, tourniquets, and disinfectants, all crucial for safe and effective blood draws.
Proper equipment maintenance and understanding its function are vital for minimizing risks and ensuring accurate specimen collection.
Safety is paramount, necessitating gloves, masks, and biohazard containers to protect both patient and phlebotomist.
Venipuncture Supplies
Essential for successful venipuncture are multi-sample needles, typically 21-23 gauge, alongside needle holders for secure attachment and control during the procedure.
Evacuated tubes, color-coded by additive, are critical for collecting specific blood components; understanding these additives – EDTA, heparin, citrate – is fundamental.
Tourniquets, applied proximal to the venipuncture site, constrict venous flow, making veins more prominent, but must be released before analysis.
Alcohol swabs are used for thorough skin disinfection, minimizing the risk of contamination, while gauze pads aid in applying pressure post-draw to halt bleeding.
Gloves, always worn, protect both the phlebotomist and the patient, adhering to universal precautions. Sharps containers are vital for safe needle disposal, preventing accidental sticks.
Safety Equipment
Paramount to phlebotomy practice is comprehensive safety equipment, beginning with personal protective equipment (PPE) like disposable gloves, crucial for barrier protection.
Face shields or masks safeguard against potential splashes or aerosolized blood, minimizing exposure risks. Lab coats provide an additional layer of protection for clothing.
Sharps containers, puncture-resistant and leak-proof, are non-negotiable for the immediate disposal of used needles and other sharp objects, preventing injuries.
Biohazard bags are essential for containing contaminated materials, ensuring proper handling and disposal according to regulations. Spill kits are vital for managing accidental blood spills.
Emergency kits, including first aid supplies and contact information, should be readily accessible in case of unforeseen incidents, promoting a safe work environment.
Specimen Tubes & Additives
Various specimen tubes are utilized in phlebotomy, each distinguished by its color-coded top and specific additive, influencing test results.
Lavender-top tubes contain EDTA, an anticoagulant preventing clotting, ideal for hematology tests like complete blood counts (CBCs). Blue-top tubes utilize sodium citrate, also an anticoagulant, for coagulation studies.
Red-top tubes lack additives, allowing blood to clot naturally, suitable for serum chemistry panels. Green-top tubes contain heparin, another anticoagulant, used for certain chemistry tests.
Gray-top tubes contain sodium fluoride and potassium oxalate, preserving glucose levels for glucose tolerance tests. Proper tube selection and fill volume are critical for accurate results.
Understanding additive functions and potential interferences is essential for phlebotomists, ensuring specimen integrity and reliable diagnostic information.

Understanding Anatomy & Physiology
Knowledge of human anatomy, particularly the circulatory system, is fundamental for successful and safe phlebotomy practice.
Understanding vein structure and physiological responses aids in efficient blood draws and minimizes patient discomfort.
Comprehending potential complications requires recognizing anatomical variations and physiological factors impacting blood collection.
Vein Identification & Selection
Successful venipuncture hinges on accurately identifying suitable veins. Palpation is key; feel for bouncy, resilient vessels, avoiding scarred or damaged areas.
The median cubital vein, located in the antecubital fossa, is often the first choice due to its size and stability. The cephalic and basilic veins are alternatives.
Visual inspection can supplement palpation, noting vein diameter and straightness. Avoid veins that are tortuous, rolling, or deeply embedded.
Consider patient factors like arm dominance, mastectomy history, and edema. Proper vein selection minimizes discomfort, hematoma risk, and specimen contamination, ensuring reliable results. Always prioritize patient safety and comfort during this critical step.
Remember that consistent practice and a thorough understanding of anatomical landmarks are essential for proficient vein identification.
Arm Anatomy for Phlebotomy
Understanding arm anatomy is fundamental for safe and effective phlebotomy. The antecubital fossa, containing the median cubital, cephalic, and basilic veins, is the primary venipuncture site.
Key structures include the brachial artery, which lies medial to the veins, and the median nerve, positioned superficially. Awareness of these structures prevents accidental injury.
Superficial fascia contains veins and nerves, while deeper fascia provides structural support. Muscles like the biceps brachii and triceps brachii influence vein accessibility.
Knowledge of bony landmarks – the humerus and radius – aids in locating veins. Proper anatomical understanding minimizes complications like nerve damage or arterial puncture, ensuring patient well-being and accurate specimen collection.
Consistent review of anatomical diagrams and practical application reinforce this crucial knowledge base for phlebotomists.
Common Complications & Their Causes
Phlebotomy, while routine, carries potential complications. Hematoma formation results from blood leaking into surrounding tissues, often due to insufficient vein compression post-puncture.
Nerve injury can occur from direct needle contact or hematoma compression, causing pain or numbness. Arterial puncture, though rare, presents a serious risk due to uncontrolled bleeding.
Infection, though minimized by aseptic technique, remains a concern. Fainting (syncope) is often triggered by anxiety or vasovagal response.
Hemolysis, the rupture of red blood cells, can stem from vigorous shaking or improper tube handling. Understanding these causes allows phlebotomists to implement preventative measures and respond effectively to adverse events, prioritizing patient safety.
Prompt recognition and appropriate intervention are crucial for managing these complications.
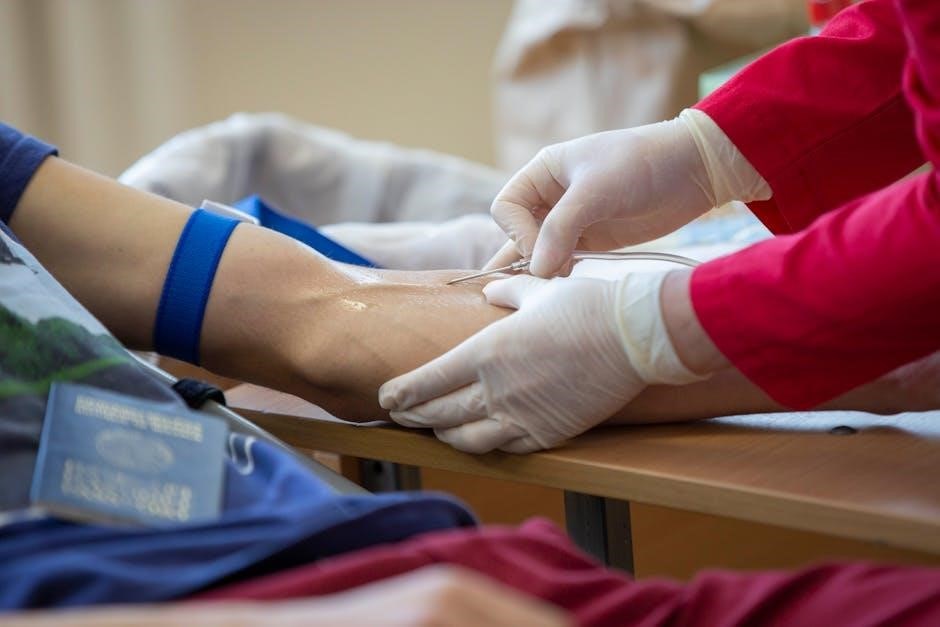
Phlebotomy Procedures: Step-by-Step
Successful venipuncture requires meticulous adherence to protocol, from patient identification to post-puncture care, ensuring accuracy and safety.
Proper technique minimizes discomfort and complications, while maintaining specimen integrity for reliable test results.
Detailed guidance is essential for mastering each step, building confidence and competence in phlebotomy practice.
Patient Identification & Preparation
Accurate patient identification is the cornerstone of safe phlebotomy practice. Always verify at least two identifiers – typically the patient’s full name and date of birth – against the requisition form and the patient’s identification band.
Confirm any allergies, especially to latex or alcohol, and document them clearly. Explain the procedure to the patient in a clear, concise manner, addressing any anxieties or concerns they may have.
Assess the patient’s arm for suitable veins, avoiding areas with hematomas, scars, or edema. Position the patient comfortably and ensure adequate lighting. Ask about medications, particularly anticoagulants, as they may affect bleeding time. Finally, prepare the site with an appropriate antiseptic solution, allowing it to dry completely before venipuncture.
Venipuncture Technique – Detailed Guide
Anchor the vein by gently stretching the skin below the puncture site with your non-dominant hand. Insert the needle at a 15-30 degree angle, bevel up, with a smooth, controlled motion.
Observe for a flash of blood in the hub of the needle, indicating successful vein entry. Advance the needle slightly, then secure the collection tube to the hub adapter. Allow the tube to fill completely, inverting gently as needed to mix any additives.
Release the tourniquet before removing the needle to prevent hematoma formation. Apply gentle pressure to the puncture site with a sterile gauze pad while withdrawing the needle. Activate safety features immediately and dispose of the needle properly.
Post-Puncture Care & Patient Monitoring
After needle removal, maintain firm pressure on the puncture site for at least three to five minutes, ensuring complete hemostasis. Instruct the patient to continue applying pressure and avoid bending their arm for an extended period.
Observe the patient for any signs of adverse reactions, such as dizziness, nausea, or continued bleeding. Ask about any discomfort or pain at the puncture site. Provide a bandage and offer assistance if needed.
Document any complications or unusual observations in the patient’s record. Reinforce the importance of following any post-procedure instructions provided. Ensure the patient feels comfortable and safe before dismissing them.

Specialized Collection Techniques
Certain patient populations require modified phlebotomy approaches, including pediatric, geriatric, and those with difficult venous access.
Adapting techniques ensures patient safety, minimizes discomfort, and maximizes collection success in unique circumstances.
Pediatric Phlebotomy
Pediatric phlebotomy demands a specialized approach, prioritizing patient comfort and minimizing trauma. Children often experience heightened anxiety and fear regarding medical procedures, necessitating gentle communication and a calm demeanor from the phlebotomist.
Preparation is key; explaining the procedure in age-appropriate terms, using distraction techniques (toys, stories), and involving parents or guardians can significantly reduce distress. Site selection differs; smaller gauge needles and shallow punctures are preferred.
Capillary collection (heel sticks or fingersticks) is frequently utilized for infants and toddlers, while venipuncture is reserved for older children when possible. Proper immobilization and support are crucial; Post-procedure comfort measures, like bandages with fun designs, can further ease anxiety. Always adhere to established pediatric guidelines and protocols.
Geriatric Phlebotomy
Geriatric phlebotomy requires sensitivity and adaptation due to age-related physiological changes. Elderly patients often have fragile veins, decreased skin elasticity, and potential underlying medical conditions impacting blood collection.
Techniques must be modified; using smaller gauge needles, vein illumination, and gentle site massage can aid in successful venipuncture. Prolonged tourniquet application should be avoided to prevent hematoma formation. Patient positioning is vital for comfort and safety.
Communication is paramount; explain the procedure clearly and patiently, addressing any concerns. Be mindful of cognitive impairments and involve caregivers when necessary. Post-puncture pressure must be maintained for a longer duration due to slower clotting times. Prioritize patient well-being and minimize discomfort throughout the process.
Difficult Draws & Alternative Sites
Encountering difficult draws is common in phlebotomy, requiring patience and a systematic approach. Factors include collapsed veins, rolling veins, and patient anxiety. Attempting multiple punctures at the same site should be avoided to minimize trauma.
Alternative sites, such as the hand or wrist, may be considered when antecubital veins are inaccessible. However, these sites carry increased risks of complications like nerve damage and hematoma. Foot venipuncture is generally avoided unless absolutely necessary.
Proper technique, vein selection, and patient reassurance are crucial. Utilizing vein visualization aids and applying appropriate pressure can improve success rates. Document all attempts and any complications encountered. Always prioritize patient safety and comfort when navigating challenging draws.
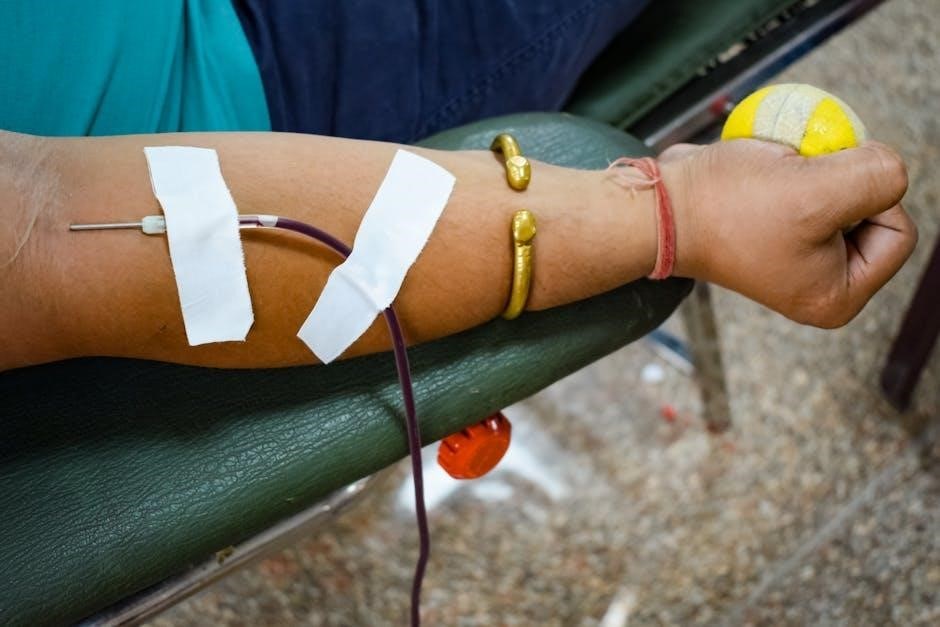
Quality Control & Safety Protocols
Maintaining specimen integrity, adhering to infection control, and prioritizing needle stick safety are vital for accurate results and patient wellbeing.
Rigorous protocols minimize errors, prevent contamination, and protect both phlebotomists and patients from potential hazards during procedures.
Consistent application of these standards ensures reliable lab data and a safe healthcare environment for everyone involved.
Specimen Labeling & Handling
Proper specimen labeling is absolutely critical to avoid errors and ensure patient safety. Each tube must be accurately labeled at the bedside, immediately after collection, with the patient’s full name, date of birth, medical record number, date, and time of collection, and the phlebotomist’s initials.
Handling specimens correctly prevents contamination and maintains sample integrity. Tubes should be gently mixed according to additive-specific guidelines – avoid vigorous shaking which can cause hemolysis.
Transport specimens promptly to the laboratory, following established temperature and time constraints. Utilize appropriate transport containers to prevent leakage or breakage. Document any deviations from standard procedures. Accurate labeling and careful handling are foundational to reliable diagnostic testing and patient care.
Infection Control & Universal Precautions
Adhering to strict infection control protocols and universal precautions is paramount in phlebotomy to protect both the phlebotomist and the patient. Treat all blood and body fluids as potentially infectious, regardless of known status.
Essential practices include thorough hand hygiene – washing with soap and water or using an alcohol-based hand sanitizer – before and after each patient encounter. Always wear appropriate personal protective equipment (PPE), such as gloves, and potentially gowns and face shields.
Proper disposal of sharps in designated containers is crucial. Disinfect work surfaces regularly. Understand and follow institutional policies regarding infection control and exposure incidents. Consistent application of these precautions minimizes the risk of transmission of bloodborne pathogens.
Needle Stick Safety & Reporting
Needle stick injuries are a significant concern in phlebotomy, posing a risk of exposure to bloodborne pathogens. Employing safety-engineered devices – like retractable needles – is vital to minimize these incidents. Never recap, bend, break, or hand-manipulate used needles.
Immediately after a needle stick, wash the wound thoroughly with soap and water. Report the incident to your supervisor, even if no injury is visible. Post-exposure prophylaxis may be necessary, depending on the source patient’s status.
Complete an incident report detailing the circumstances of the injury. Follow institutional protocols for medical evaluation and follow-up testing. Proactive safety measures and prompt reporting are essential for protecting your health and preventing future occurrences.

Legal & Ethical Considerations
Phlebotomy demands strict adherence to legal standards, including patient privacy laws like HIPAA, and ethical principles of respect and confidentiality.
Informed consent is crucial before any procedure, ensuring patients understand the risks and benefits, and have the right to refuse.
Accurate documentation is legally required, providing a clear record of all procedures and patient interactions for accountability.
Patient Confidentiality (HIPAA)
The Health Insurance Portability and Accountability Act (HIPAA) is paramount in phlebotomy practice, safeguarding Protected Health Information (PHI).
PHI encompasses any individually identifiable health information, including patient names, dates of birth, social security numbers, and medical records.
Phlebotomists must maintain strict confidentiality, limiting access to PHI to authorized personnel only. Discussing patient information in public areas or with unauthorized individuals is a direct HIPAA violation.
Proper handling of specimen labels, request forms, and electronic health records is essential. Secure storage and disposal of documents containing PHI are also critical.
Violations of HIPAA can result in significant fines and legal penalties, emphasizing the importance of comprehensive training and adherence to privacy protocols. Understanding patient rights regarding their health information is also key.
Informed Consent
Informed consent is a fundamental ethical and legal principle in healthcare, including phlebotomy. It ensures patients understand the procedure, its risks, and benefits before agreeing to blood collection.
Phlebotomists are responsible for explaining the process in clear, understandable language, addressing any patient questions or concerns. This includes detailing potential discomfort, like brief pain or bruising.
While explicit written consent isn’t always required for routine venipuncture, verbal consent is essential. For specialized collections or research-related draws, formal written consent is typically mandated.
Patients have the right to refuse blood collection without penalty. Respecting this autonomy is crucial. Documenting the consent process, even verbally obtained, is good practice.
Failure to obtain informed consent can lead to legal repercussions and ethical breaches, highlighting the importance of patient education and respect for their choices.
Documentation & Record Keeping
Meticulous documentation is a cornerstone of responsible phlebotomy practice. Accurate records ensure patient safety, facilitate effective communication among healthcare professionals, and provide a legal defense if needed.

Phlebotomists must document the date, time, and type of blood draw, the specimen tubes collected, and any difficulties encountered during the procedure; Patient identifiers must be verified and recorded correctly.
Any adverse reactions experienced by the patient, such as fainting or hematoma formation, must be documented immediately, along with any interventions taken.
Record keeping should adhere to HIPAA guidelines, maintaining patient confidentiality. Electronic health records (EHRs) are increasingly common, requiring proficiency in their use.
Complete and accurate documentation demonstrates professional accountability and contributes to the overall quality of patient care, safeguarding both the patient and the phlebotomist.
Troubleshooting Common Issues
Addressing challenges like hematoma, fainting, or hemolysis requires quick thinking and proper technique to ensure patient well-being and sample integrity.
Effective problem-solving minimizes errors and maintains quality control during the blood collection process, vital for accurate results.
Hematoma Formation
Hematoma formation, a common complication, occurs when blood leaks from the vein into surrounding tissues during or after venipuncture. Several factors contribute, including inadequate vein stabilization, excessive probing, or continued pressure after needle removal.
Prevention is key; proper technique, firm vein stabilization, and avoiding multiple punctures significantly reduce risk. Applying sufficient pressure to the puncture site immediately after needle withdrawal is crucial – typically for at least 3-5 minutes, even longer for patients on anticoagulants.
If a hematoma begins to form, immediately stop the bleeding, elevate the arm, and apply a cold compress. Document the incident accurately, noting the size and location of the hematoma. Patient education regarding post-puncture care is also essential to minimize further complications.
Fainting & Vasovagal Syncope
Fainting, or vasovagal syncope, is a sudden, temporary loss of consciousness often triggered by the physiological response to venipuncture. It results from a drop in heart rate and blood pressure, reducing blood flow to the brain. Anxiety, pain, or prolonged standing can exacerbate this reaction.
Recognizing pre-syncope signs – pallor, sweating, dizziness, nausea – is vital. Immediately stop the procedure, protect the patient from injury, and lower their head between their knees. Ensure adequate ventilation and reassure the patient.
Preventative measures include patient comfort, distraction techniques, and encouraging deep breathing. Post-procedure, advise patients to remain seated for a few minutes and hydrate adequately; Document any fainting episodes thoroughly, including interventions taken.
Hemolysis & Specimen Rejection
Hemolysis, the rupture of red blood cells, compromises specimen integrity, leading to inaccurate lab results. It can occur during collection, processing, or transport due to vigorous shaking, improper tube mixing, or small needle size. Visual inspection reveals a reddish or pinkish hue to the plasma or serum.
Specimen rejection happens when samples don’t meet laboratory standards – incorrect labeling, insufficient quantity, or hemolysis are common causes. Rejection delays diagnosis and necessitates recollection, impacting patient care and workflow.
Preventing hemolysis involves gentle handling, appropriate tube order of draw, and avoiding prolonged tourniquet time. Proper labeling and adequate sample volume are crucial to avoid rejection. Thorough documentation of any issues is essential.
Resources & Further Learning
Numerous phlebotomy certification programs are available, enhancing skills and career prospects. Several excellent books and websites offer comprehensive learning materials.
Continuing education ensures staying current with evolving techniques and safety protocols within the phlebotomy field.
Phlebotomy Certification Information
Several nationally recognized agencies offer phlebotomy certification, including the American Society for Clinical Pathology (ASCP), the National Healthcareer Association (NHA), and the American Medical Technologists (AMT).
Certification typically requires completing an accredited phlebotomy training program and passing a comprehensive examination. Accredited programs ensure adherence to standardized curriculum guidelines, covering essential phlebotomy techniques, safety protocols, and medical terminology.
The ASCP offers the PBT (Phlebotomy Technician) certification, widely respected in the healthcare industry. NHA provides the Certified Phlebotomy Technician (CPT) credential, while AMT offers the Registered Phlebotomy Technician (RPT) certification.
Choosing the right certification depends on employer preferences and career goals. Certification demonstrates competency, enhances job opportunities, and often fulfills state licensing requirements where applicable. Always verify the accreditation status of any training program before enrolling.
Recommended Phlebotomy Books & Websites
“Phlebotomy Essentials” by Ruth E. McCall is a widely used textbook, offering comprehensive coverage of phlebotomy principles and procedures. “Clinical Phlebotomy: A Course Manual” by Jean Gallin and Mary Houser provides detailed instructions and practical exercises.
For online resources, the ASCP website (https://www.ascp.org/) offers valuable information on certification and best practices. The NHA website (https://www.nhanow.com/) provides details about their CPT credential and study materials.
LabSkills (https://www.labskills.com/) offers interactive modules and practice quizzes. Additionally, many free phlebotomy resources, including practice exams and study guides, are available online, but verify their accuracy and credibility before use.
Remember to supplement textbook learning with hands-on practice and clinical experience for optimal skill development.
Continuing Education Opportunities
Maintaining current certification often requires ongoing education. The ASCP (American Society for Clinical Pathology) offers numerous continuing education modules online, covering topics like updated safety protocols and new collection techniques.
The National Healthcareer Association (NHA) also provides continuing education opportunities specifically tailored for Certified Phlebotomy Technicians (CPTs). Many hospitals and healthcare facilities sponsor in-service training sessions.
Online platforms like Meditec and ProSolutions University offer accredited phlebotomy CE courses. Consider attending workshops or seminars at professional conferences to network and learn from experts. Regularly reviewing updated guidelines from CLSI (Clinical and Laboratory Standards Institute) is crucial.
Staying informed ensures competency and provides the best possible patient care.